About a year ago, a lady from a neighbouring country urgently flew to see me. She came to discuss the CT scan results of a VIP (very important personality). The CT scan clearly stated that this VIP had tumours in his lungs and liver. His doctor suggested immediate surgery. This lady wanted my advice.
Just to be on the safe side, I suggested that it might be a good idea to know the extent of possible metastases – if at all there is any spread – before undergoing surgery. Towards this end, I suggested that he goes for a PET scan. At that time, my impression was that the PET is the state-of-the-art imaging procedure. It is more accurate and reliable than the CT scan.
After a few days, I was informed by phone that the PET done did not show any malignancy – no cancer! Nevertheless, I hesitated to believe the result. At that time, I “interpreted” the message differently. I had the impression that this VIP wanted to avoid any dealing with me and therefore the only polite “save face” strategy was to tell me that there was no cancer. So he does not need my help anymore!
Some months later, I got to know through another person that this VIP had undergone a liver surgery. This planted the first seed of doubt in my mind about the reliability of PET scan.
Patient from Kelantan
In October 2011, I received a fax from a patient in Kelantan. This 47-year-old male patient did a CT scan on 22 August 2011. The results indicated:
- Three well-defined heterogenously hypodense small liver lesions in segments 2, 7 and 8. The largest in segment 2 measuring 0.7 x 1.0 cm. Foci of non-enhancing calcification seen in segment 8 with no mass effect, likely to represent old infection.
- Small, well-defined lung nodule seen in the anterior segment of right upper lobe of 0.3 cm in diameter. A small pleural-based nodule is also seen in the posterior segment of left lower lobe measuring 0.3 cm in diameter.
- Well-defined small sclerotic bony lesions see in at right acetabulum, left ilium and left neck of femur likely to represent bony island. Multilevel degenerative of the visualized spine.
Impression: Known case of sigmoid colon carcinoma with liver and lung metastases.
This same patient went to do a PET scan in Kuala Lumpur on 5 October 2011. The PET scan result indicated the following:
- There is normal uptake in all the organs examined, in particular the colon, liver, lungs, lymph nodes, spleen, pancreas, kidneys, adrenal glands, brain and bones. There is no pleural effusion or ascites.
Impression: No malignant lesion is detected.
This was the second alarm bell. However, I did not take this episode to heart because the patient did not come to see me personally and I did not get to see the images of both the scans. As such I do not have any “solid” evidence to back up what I say – although I did have the faxed reports of both the procedures.
Patient from Penang
The third alarm bell – on 5 February 2012. A man came to our Centre with the medical reports of his wife who has ovarian cancer. She underwent surgery – TAHBSO (Total abdominal hysterectomy with bilateral salpingo-oophorectomy) – on 15 September 2010. This time I had the opportunity to examine the images of both the PET and CT scans.
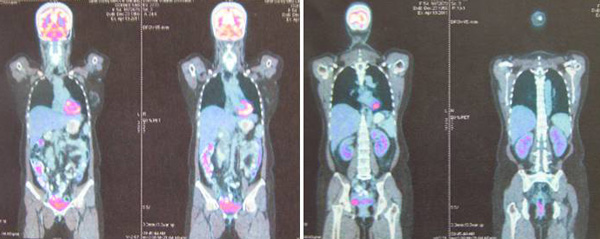
Six months after the surgery, a PET scan was done at a private hospital in Selangor on 19 April 2011.
Technique: PET scan was performed from the vertex of the skull to the thighs after intravenous administration of 8.5 mCi of F-18 Fluorodeoxyglucise (FDG). Oral gastrograffin, oral bromazepam and intra-venous lasix were given. Fasting blood glucose – 6.9 mmol/l/
Findings:
- Head – There is normal physiological localization of the FDG in the cerebrum and the cerebellum. The uptake and the distribution of the radiotracer in the posterior nasopharyngeal tissue, salivary gland and tonsils are within normal physiological limits.
- Neck –The thyroid gland displaces normal FDG upake. There is no FDG avid cervical lymphadenopathy.
- Thorax – Normal FDG uptake is seen in both breasts. There is no FDG avid axillary lymphadenopathy, bilaterally. There is no FDG avid mediastinal lymphadenopathy. Thre is no pleural effusion seen.
- Abdomen – There is no suspicious FDG avid lesion see in the liver. U[take and distribution of the radiotracer in the gallbladder, spleen, adrenals, pancreas, kidneys and bowels are within normal physiological limits. There is no FDG avid abdominal lymphadeopathy. Ascites is not present.
- Pelvis – TAHBSO noted. There is no definite abnormal FDG lesion seen in the pelvic floor and vaginal stump. There are some superficial subcentimetre size non-FDG avid inguinal nodes which are likely to be reactive nodes. There is no FGD pelvic lymphadenopathy.
- Musculoskeletal – There is symmetrical FDG avid activity seen in the acromioclavicular joints bilaterally, probably due to imflammation. There is no suspicious FDG avid lesion seen in the visualized skeleton.
Conclusion;
- There is no evidence of residual hypermetabolic disease in the vaginal stump and pelvic floor.
- There is no evidence of hypermetabolic loco-regional or distant metastatic disease at present.
- Although there is no evidence of macroscopic disease at present, the presence of microscopic disease cannot be excluded.
The above report was signed by the Consultant Nuclear Medicine Physician.
Three months later, 25 July 2011, this same lady did an ultrasound of her abdomen and pelvis at the same private hospital in Selangor. The results indicated:
- Mild ascites is seen.
- A thick layer of lobulated parietal pleural masses are seen subdiaphragmatically, around the liver edges superiorly and laterally.
- It measures up to 6 x 3.5 cm around segment 8 of the liver and 4.5 x3.7 cm superior to segment 2.
- Intrahepatically, a hypoechoic nodule measuring 15 mm is noted in segment 3.
- There are also intraperitoneal mesenteric deposit, measuring up to 3.6 x 2.8 cm in the right lumbar territory.
- The uterus and ovary absent.
Impression: Extensive intraperitoneal metastases with ascites. Significant progression of the metastasis is seen.
On 16 November 2011, a CT scan of this same lady was done at a private hospital in Penang. The results indicated:
- Extensive lobulated hypodense mass noted in the peritoneum and mesentery of upper abdomen.
- The mass measured approximately 25 to 65 mm in diameter each.
- The mass creep in between the diaphragm and the dome of the liver with marked subcapsular compression of liver.
- Masses also noted in the lesser sac and the para-splenic space.
- Moderate ascites.
- Previous hysterectomy.
Impression: In view of the clinical history, features are consistent with relapsed of carcinoma of ovary with extensive peritoneal and omental metastasis.
Let me end with another story. There was this man who had stomach cancer. After surgery he came to seek our help and was started on the herbs. According to him, he felt good. He liked gardening and used to bring a lot of hot “cabai burung” whenever he came to our centre. He knew that I like hot chilly. One day this patient came and told us that he just had just done a scan and his doctor told him he had no more cancer – everything was clean. So he did not want to take any more herbs – after all the doctor said he was already cured! Although I did warn him that there is no such thing as a cure! No, his doctor’s words were more powerful and after all this was what every cancer patient wants to hear anyway.
A few months later, someone showed me his obituary in the newspaper. Besides learning that he was dead, I also learned that this man was a Datuk – a titled, respected personality in the community.
From the above stories, I learned that we can cause grave danger to patients by telling them things that they only want to hear. Or sending them for test that can give results that they are looking for – of course, the more high-tech the equipment involved, the more convincing it would be. So danger is not only confined to giving them the “wrong kind” of medication – the more toxic the more dangerous.
In this case the lady patient above had a choice – to believe that she had NO cancer after her surgery. What a great relief and welcoming news when the high tech state-of-the art technology similarly confirmed this belief. The lady also had another choice – to believe that surgery did not in any way cure her cancer and actually there were a lot more of the cancer cells left behind after the surgery! High tech gadget was unable to detect that but intuition and plain old-fashion experience is able to decipher that possibility.
Incidentally, while writing this article, I was also reading this humorous, oft-quoted all-time favorite book written by Dr. Oscar London, M.D., the pseudonym of an internist practising in Berkeley, California.






You must be logged in to post a comment.