Yeong Sek Yee & Khadijah Shaari
To understand more about the radiation risks from medical imaging, we recommend that you read the following articles posted in the Internet. Just Google topics like the dangers of medical/diagnostic tests, etc, etc. There are plenty of materials to read. Here are some examples.
1. Medical Radiation Soars, With Risks Often Overlooked
Radiation, like alcohol, is a double-edged sword. Radiation can reveal hidden problems, from broken bones and lung lesions to heart defects and tumors. But it also has a potentially serious medical downside: the ability to damage DNA and, 10 to 20 years later, to cause cancer. CT scans alone, which deliver 100 to 500 times the radiation associated with an ordinary X-ray and now provide three-fourths of Americans’ radiation exposure, are believed to account for 1.5 percent of all cancers that occur in the United States.
Although the cancer-causing effects of radiation are cumulative, no one keeps track of how much radiation patients have already been exposed to when a new imaging exam is ordered. Even when patients are asked about earlier exams, the goal is nearly always to compare new findings with old ones, not to estimate the risks of additional radiation.
Read more: http://well.blogs.nytimes.com/2012/08/20/medical-radiation-soars-with-risks-often-overlooked/?utm_source=twitterfeed&utm_medium=twitter
2. Radiation Risks from Medical Imaging
The FDA has put forward its plan to reduce unnecessary radiation exposure from CT scans, nuclear medicine studies, and fluoroscopy.
An individual’s chance of getting cancer from a single scan is small. But because the scans are so widely used, they cause a considerable amount of harm. One study estimated that the CT scans performed in 2007 are related to some 29,000 future cancers.
What are these tests? What are their risks? When do the tests’ benefits outweigh their risks? Here are WebMD’s answers to these and other questions.
How much radiation does a person get from medical imaging studies?
- Getting a CT scan gives a patient as much radiation as 100 to 800 chest X-rays.
- Getting a nuclear medicine study exposes a patient to as much radiation as 10 to 2,050 chest X-rays.
- Getting a fluoroscopic procedure exposes a patient to as much radiation as 250 to 3,500 chest X-rays.
Moreover, doctors may prescribe scans that aren’t medically justified. And since risk from radiation exposure accumulates over a lifetime, certain scans may not be appropriate for people who’ve already had a lot of scans.
Read more: http://www.medicinenet.com/script/main/art.asp?articlekey=114953
3. Dangers of Medical Imaging Tests and Procedures
Exposure to medical imaging radiation is a concern in both adults and children. However, radiation exposure in children is of a greater concern because they are more sensitive to radiation than adults. In addition, children have longer life expectancy than adults. With repeated exposure or accumulated exposure to radiation, children may be more likely to develop health problems in the future.
Life time risk of developing cancer increases when a patient undergoes more frequent X-ray exams and at larger doses, according to the FDA. Women who are exposed to the radiation may have higher lifetime risk for developing radiation-associated cancer than men after receiving the same exposures at the same ages.
While experts believe that the risk of developing cancer with radiation exposure is relatively small, radiation exposure through these medical imaging tests should never be taken lightly.
Read more: http://voices.yahoo.com/dangers-medical-imaging-tests-procedures-5452681.html?cat=5
4. A Closer Look: The Downside of Diagnostic Imaging
CT and nuclear medicine tests do have a downside, however: they deliver doses of ionizing radiation from 50 to over 500 times that of a standard x-ray, such as a chest x-ray or mammogram. Scientists have raised concerns that such large doses of radiation plus the widespread and increasing use these diagnostic procedures may, in a small but significant way, pose a cancer risk in the general population.
“The use of CT in particular has gone up dramatically, and we’ve drastically lowered the threshold for using it,” said Dr. Rebecca Smith-Bindman, a visiting research scientist with NCI’s Radiation Epidemiology Branch (REB). “There’s a general belief that if you get a CT scan, you must be reasonably sick and must really need it. This is no longer true, and we are increasingly using CT scans in patients who are not that sick. There’s been drift not only in how often we use it but in how we use it.”
“We’ve only talked about the benefits of CT for the past 20 years, without considering any potential harm” she continued.
Research estimated that approximately 29,000 future cancers could be related to CT scans performed in the United States in that year alone, with women being at higher risk than men. About 35 percent of these cancers were projected to be related to scans performed in patients 35 to 54 years old, and 15 percent related to scans performed in children younger than 18.
The medical community has proposed many ways to reduce radiation exposure from diagnostic medicine without negatively impacting the quality of patient care:
- Reduce the number of CT exams by using other technologies (such as ultrasound or MRI) in cases where they would provide equal diagnostic quality.
- Limit the use of CT in healthy patients who would obtain little benefit (such as whole-body CT screening).
- Limit the use of repeat CT surveillance of patients in whom a diagnosis has already been made, when repeat scanning would lead to little change in their treatment.
- Track and collect information on radiation exposure for individual patients
Read more: http://www.cancer.gov/aboutnci/ncicancerbulletin/archive/2010/012610/page8
5. Ionizing Radiation Exposure with Medical Imaging
Medical diagnostic procedures used to define and diagnose medical conditions are currently the greatest manmade source of ionizing radiation exposure to the general population. The risks and benefits of radiation exposure due to medical imaging and other sources must be clearly defined for clinicians and their patients.
Radiation damages the cell by damaging DNA molecules directly through ionizing effects on DNA molecules or indirectly through free radical formation. A lower dose delivered through a long period of time theoretically allows the body the opportunity to repair itself. Radiation damage may not cause any outward signs of injury in the short term; effects may appear much later in life.
Medical ionizing radiation has great benefits and should not be feared, especially in urgent situations. Obviously, using the lowest possible dose is desired. In fact, a central principle in radiation protection is “as low as reasonably achievable.” Therefore, the prescribing physician must justify the examination and determine relevant clinical information before referring the patient to a radiologist. Indications and decisions should reflect the possibility of using non-ionizing radiation examinations, such as MRI or ultrasonography.
Repetition of examinations should be avoided at other clinics or sites.
The International Commission on Radiological Protection (ICRP) estimates that the average person has an approximately 4-5% increased relative risk of fatal cancer after a whole-body dose of 1 Sv.
X-rays (including CT scans) should be ordered judiciously. An article in the New England Journal of Medicine notes that the evidence is “convincing” that the radiation dose from CT scans can lead to cancer induction in adults and “very convincing” in the case of children. Clinicians need to realize that doses from a typical CT scan can range from 6-35 times higher than the dose of a standard chest x-ray examination.
Read more: http://emedicine.medscape.com/article/1464228-overview#a30
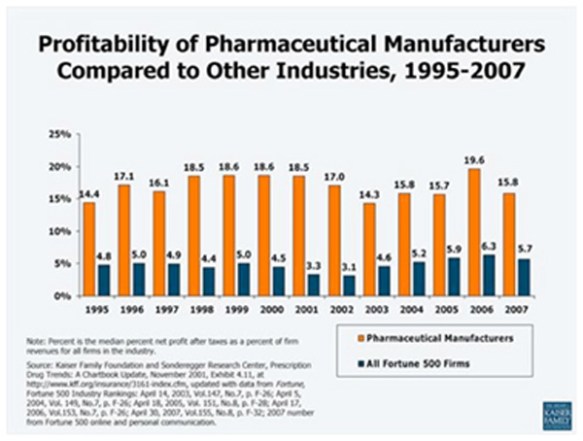
6. Doctors Order More Tests when They Benefit Financially: Ask If You Really Need that Test Your Doctor Ordered
Researchers from the Institute for Technology Assessment at the Massachusetts General Hospital Department of Radiology found that there was no mistaking that diagnostic imaging tests were being ordered far more than they deemed necessary. The question that begs to be answered is, “why?”
Many doctors referred their patients to imaging centers that were affiliated with their practice, or were even done by the doctor’s own staff. When a physician has such a close relationship with the provider conducting the imaging study, there is the possibility that the physician will benefit financially from ordering additional imaging studies.
Read more: http://voices.yahoo.com/doctors-order-more-tests-they-benefit-financially-631960.html?cat=5
7. Radiation Danger from CT and PET Scans
A recent study in the New England Journal of Medicine has found a significant link between radiation exposure and imaging procedures such as CT and PET scans. The use of such technologies has grown from just 3 million in 1980 to 67 million in 2006, and has contributed, some estimate, to upwards of 2% of fatal cancer cases.
Studies have shown that there is little consumer understanding of the risks involved in being subject to such procedures.
Dr. Harlan M. Krumholz proffers that the use of CT scans is increasing because they have become part of our culture. “People use imaging instead of examining a patient; they use imaging instead of talking to the patient,” (New York Times, Study Finds Radiation Risk for Patients, August 27, 2009). For these reasons, imaging technologies have become a common diagnostic tool even when they are not required.
Read more: http://blog.hcfama.org/2009/08/27/radiation-danger-from-ct-and-pet-scans/
8. Study Finds Radiation Risk for Patients
At least four million Americans under age 65 are exposed to high doses of radiation each year from medical imaging tests, according toa new study in The New England Journal of Medicine. About 400,000 of those patients receive very high doses, more than the maximum annual exposure allowed for nuclear power plant employees or anyone else who works with radioactive material.
Dr. Rita Redberg, a cardiologist and researcher at the University of California, San Francisco, who has extensively studied the use of medical imaging, said it would probably result in tens of thousands of additional cancers. It’s certain that there are increased rates of cancer at low levels of radiation, and as you increase the levels of radiation, you increase cancer.
Dr. Reza Fazel, a cardiologist at Emory University, said the use of scans appeared to have increased even from 2005 to 2007, the period covered by the paper. “These procedures have a cost, not just in terms of dollars, but in terms of radiation risk.”
Read more: http://www.nytimes.com/2009/08/27/health/research/27scan.html?_r=0
9. Radiation Exposure from Medical Diagnostic Imaging Procedures
Ionizing radiation is used daily in hospitals and clinics to perform diagnostic imaging procedures.
Which types of diagnostic imaging procedures use radiation?
• In x-ray procedures, x rays pass through the body to form pictures on film or on a computer or television monitor, which are viewed by a radiologist. If you have an x-ray test, it will be performed with a standard x-ray machine or with a more sophisticated x-ray machine called a CT or CAT scan machine.
• In nuclear medicine procedures, a very small amount of radioactive material is inhaled, injected, or swallowed by the patient. If you have a nuclear medicine exam, a special camera will be used to detect energy given off by the radioactive material in your body and form a picture of your organs and their function on a computer monitor. A nuclear medicine physician views these pictures. The radioactive material typically disappears from your body within a few hours or days.
Do magnetic resonance imaging (MRI) and ultrasound use radiation?
MRI and ultrasound procedures do not use ionizing radiation. If you have either of these types of studies, you are not exposed to radiation.
There is no conclusive evidence of radiation causing harm at the levels patients receive from diagnostic xray exams. Although high doses of radiation are linked to an increased risk of cancer, the effects of the low doses of radiation used in diagnostic imaging are not known.
Read more: https://hps.org/documents/meddiagimaging.pdf
10. Radiation Risk of Medical Imaging for Adults and Children
Which kinds of tests are associated with Ionising radiation and which ones are not?
1. X-rays
X-rays are ionising radiation produced by equipment used in the following types of procedures:
- Computed tomography (CT)
- Fluoroscopy (where the image produced by the X-ray beam is made into a moving picture on a TV screen
- Plain radiology/X-ray film, digital and computed radiography (see Plain Radiography / X-rays)
- Mammography (see Diagnostic Mammography)
- The radiation exposure from having an X-ray, fluoroscopy, mammography or CT examination only occurs while the machine is on.
2. Magnetic resonance imaging (MRI)
MRI uses strong magnetic fields and radio waves to produce images. It does not use ionising radiation (see Magnetic Resonance Imaging (MRI)).
3. Ultrasound
Ultrasound uses high frequency sound waves that the human ear cannot detect to obtain imaging information (see Ultrasound).
4. Nuclear medicine
Nuclear medicine is a medical specialty that involves the administration of a small amount of a radioactive material into the patient. The patient becomes weakly radioactive for a short time and images are made from the radiation given off from the patient (see Nuclear Medicine).
How do I decide whether the risks are outweighed by the benefits of exposure to X-radiation when I have a radiology test or procedure?
- Ask your doctor about the procedure and how it will help to provide information about your symptom or the presence of disease or injury.
- Ask your doctor about the risks of the procedure and what the risks would be of not having the procedure, i.e. if your doctor needs the information in order to identify and plan the most appropriate treatment.
While there is a small risk of harm from ionising radiation, there could be a greater risk of not having the information, e.g. failure to detect potentially serious disease that may be easily treated at an early stage but harder to treat or incurable if detected later.
It may also be as beneficial to you to confirm the absence of disease or injury as it is to confirm its diagnosis.
Read more: http://www.insideradiology.com.au/pages/view.php?T_id=57
11. Radiation in Medical Imaging Has Its Risks
Almost all medical procedures, including imaging procedures that use radiation, have risks associated with them. Physicians and patients should carefully consider the potential benefits and the risks when considering the use of imaging techniques that involve radiation.
Here are some things for healthcare providers to consider when deciding whether or not an imaging procedure that uses medical radiation is the right choice.
- What is the purpose of the procedure? For example, is it to arrive at a diagnosis, assess treatment response, or is it preventive screening?
- Are there alternative imaging procedures that could accomplish the same goal without medical radiation, such as ultrasound or magnetic resonance imaging?
- What are the risks of not having the imaging procedure done?
- How old is the patient? The risks for pediatric and adolescent patients may be different than for adults.
- Is the patient pregnant, possibly pregnant, or breastfeeding?
- What other procedures is the patient likely to undergo during this workup?
- What is this person’s radiation exposure from previous medical procedures? For example, has the person undergone multiple CT or nuclear medicine scans in the past?
- What is this person’s occupational exposure to radiation, if any?
- Will the imaging exam be performed on low-dose equipment?
The standard unit of measure for radiation absorbed by an individual is called the “Sievert,” or Sv (sometimes identified by a smaller unit called the “millisievert,” or mSv). Common medical imaging tests such as X-rays or mammograms generally expose patients to a radiation dose of less than 1 mSv.
Other procedures using CT, nuclear stress tests, or fluoroscopy-guided exams often involve radiation in the range of 5-40 mSv.
A single exposure at these diagnostic levels may not pose much risk to the patient. But when a patient has numerous tests over a period of time, the cumulative exposure may raise the level of risk. To minimize cumulative exposure, physicians should determine whether a procedure using medical radiation is necessary to achieve the diagnosis or whether an alternative imaging procedure may offer the same diagnostic benefit.
Read more: http://www.gehealthcare.com/dose/medical-radiation/benefits-and-risks.html
12. How Safe or Unsafe Are Medical Imaging Procedures?
Radiation exposure is a known risk factor for cancer. Recent estimates suggest, for example, that as many as two percent of cancers could be attributed to radiation during CT scans. Although the radiation exposure from a single test is minimal, the frequency of the use of imaging tests that emit radiation continues to grow expansively, and often patients undergo repeated or multiple types of tests, thereby increasing their cumulative exposure to potentially cancer-causing radiation.
Read more: http://www.sciencedaily.com/releases/2009/08/090826191837.htm
Advice to Patients
Lately, we have noticed that certain medical centres have been urging cancer patients to perform regular CT or PET scans (some every 3 months) to “monitor” the progress of their cancer treatment. Sometimes some cancer patients think that such CT/PET scans are “treatment” itself. The medical establishment obviously have a financial benefit in urging you to perform more imaging/diagnostic procedures.
When deciding whether or not to perform further imaging/diagnostic procedures, we would advise you to seek answers to the following:
- What is the purpose of the procedure? For example, is it to arrive at a diagnosis, assess treatment response, or is it preventive screening?
- Are there alternative imaging procedures that could accomplish the same goal without medical radiation, such as ultrasound or magnetic resonance imaging?
- What are the risks of not having the imaging procedure done?
- What is your radiation exposure from previous medical procedures? For example, have you undergone multiple CT or nuclear medicine scans in the past?
Each time you are asked to do a CT Scan/PET Scan, be aware of the amount of radiation that would be bombarding your body and do remember that the radiation is accumulative i.e. it accumulates in your body, not the doctor’s body (except his wallet gets heavier). The following article is self explanatory:

































You must be logged in to post a comment.