When I woke up on the morning of 2 April 2024, Im told me that she had a dream. Ina, our cancer patient and a good friend, came to her in a dream.
In my dream, Ina was wearing a bright dress with many colors, and
everything looked bright and cheerful. I felt happy.
Chris was busy working at his computer – his back facing us.
Ina and I were happily sharing something on another computer when
she took out a cartridge and inserted it into a gadget and told me that we may have duplicates of some pictures. She said: There is no need to make copies of everything. I said something (that I cannot remember).
Then she turned to the left and picked up two babies, one on each arm and showed them to me.
I told her not to strain herself. She smiled and said it is okay.
That was when I woke up suddenly. I looked at the clock in my room – it was 7:30 a.m. I felt very afraid – my heart was very troubled. For a long while, I dared not check my handphone for fear of receiving any bad news about Ina.
There was a message in our whatsapp: Aunty passed on early this morning.
To be honest, this sad news came as no surprise. When you have metastatic cancer, we know that there is no cure. There will be a day when we need to accept that death will come. That is the final cure for cancer. But while we are still alive, let us pray that there is no suffering and we go in peace. This is the message I would like to share with you.
That same evening, Im and I went to pay our last respect to Ina and got to meet some members of her family. Although the mood was sober no one showed any feeling of desperation – everyone in the family did their best and Ina’s time was up and she left without any suffering. Amazingly after (or before?) she left Ina visited Im in her dream.
There is no denying, this is a good death.
Let me recall what happened to Ina – whom I wrote about in our book Breast Cancer – Sharing our 25 years of experience.
Her Tango with Breast Cancer
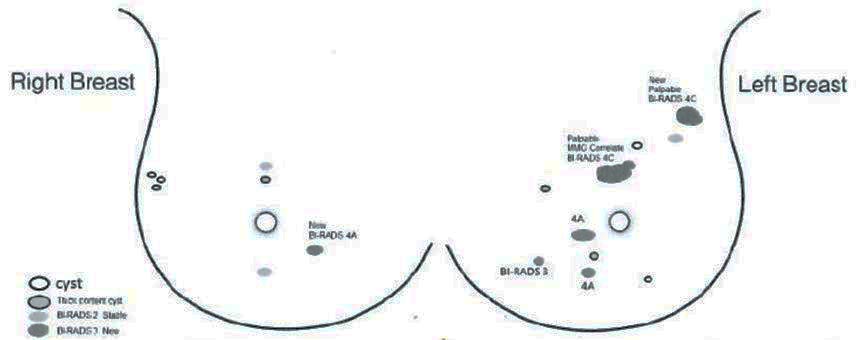
Ina was 51 years old when she was diagnosed with Stage 2 left breast cancer with nodal metastases. This was 12 years ago – around July 2012. She underwent surgery to remove the cancerous breast but refused further medical treatment – no radiation , no chemo and no tamoxifen, etc. She opted for our therapy – i. e., herbs and change of diet.
Why did she not want to go for chemo, radiotherapy, etc.? Unfortunately, Ina came from a family with cancer problems. She once told me that 50% of her family members got cancer. Both her father and mother died of cancer and she saw how they suffered. No, she would not want to go through all those tortures.
For 8 years (2012 to 2020), Ina was doing well and led a perfectly normal life. She took care of her diet very well and was serious about taking care of her health. She once told me that she hoped to live for “another 30 years”.
But it was not to be. The world was struck by the Covid-19 epidemic. During this lockdown period we did not get to see much of Ina. She was out of our radar. During this time, something was brewing up.
- Ina had her Sinovac vaccination:
- First dose: 9 July 2021
- Second dose: 30 July 2021
- Booster dose: 12 December 2021
- Her blood test results on 17 September 2022 showed “good health, nothing abnormal”, as below:
ESR = 10
Platelet count = 271
Liver function tests = all values within normal range.
Alpha fetoprotein = less than 1.3
CA 125 = 4.8 (normal)
CA 15.3 = 14.9 (normal)
CA 19.3 = 28.7 (normal)
CEA = 0.9 (normal)
- Ina was infected with Covid-19 on 25 September 2022 – in spite of the vaccination received earlier.
- Ina became breathless and came to seek our help. She was given Lung Tea. After taking Lung Tea she felt okay.
- Blood test on 10 May 2023 showed deteriorating results:
ESR = 52 High
Platelet count = 275
CA 125 = 4.7
CA 15.3 = 65.5 High
CA 19.9 = 48.8 High
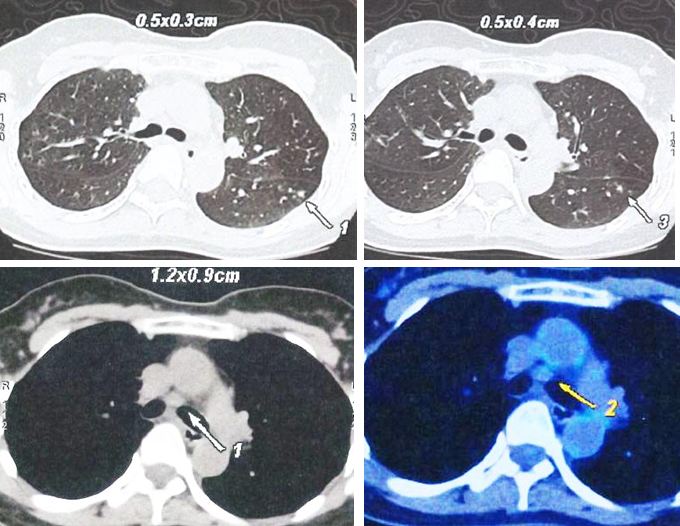
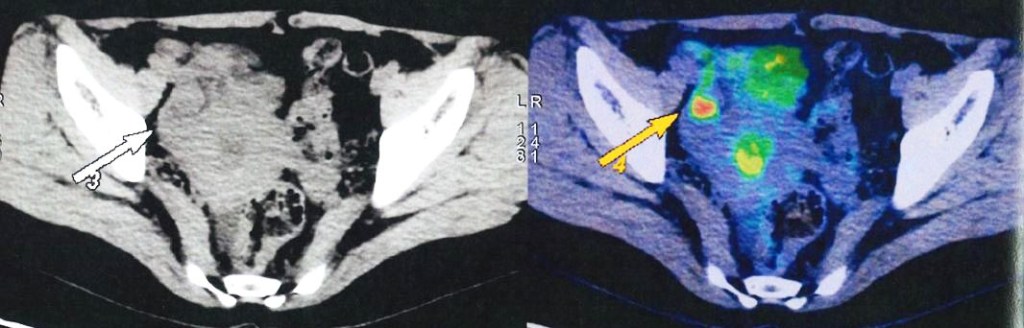
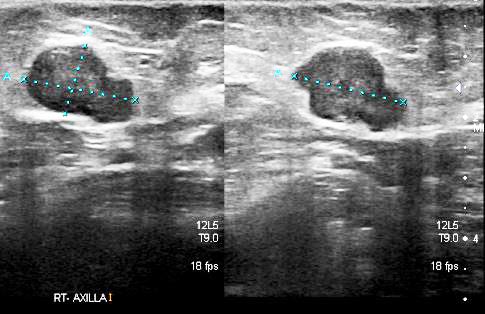
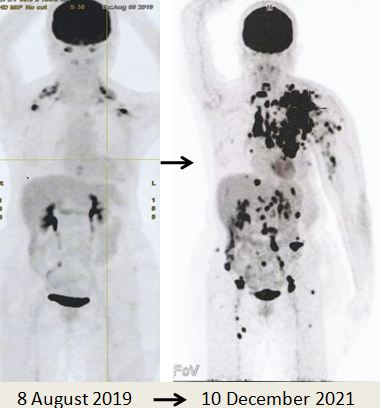
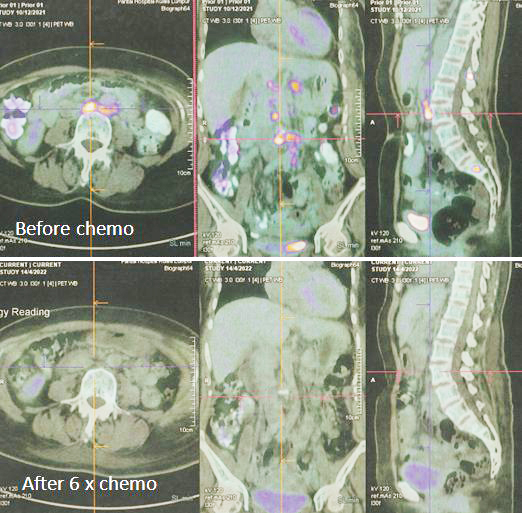
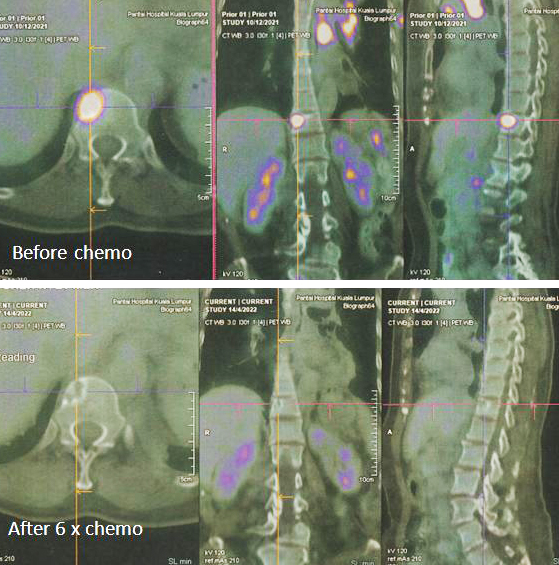
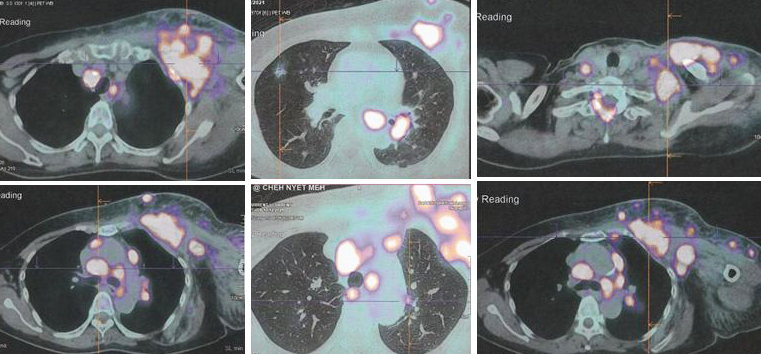
- PET scan on 14 September 2023 showed more serious condition.
- The metabolically active left lung mass with multiple neck, axillary and mediastinal nodes. Left pleura and bone lesions are likely due to primary lung malignancy.
- However, metastatic breast cancer recurrence cannot be excluded.
- Ina continued to take the lung herbs. In view of the above PET scan results (now suggesting that she might have lung cancer besides breast cancer!) I suggested that Ina seek medical opinion and help in addition to taking our herbs. Ina made it clear to me that whatever it is, she was not prepared to go for chemotherapy or radiotherapy.
- Ina still managed to lead a normal life but many times she felt breathless to the point of not being able to walk much. Another problem she faced was wind or gas in her stomach which made her uncomfortable.
- One day in early 2024, Ina, her husband, son and daughter came to our house for consultation – What to do now? This was my advice to Ina.
- Yes, by all means go and consult the doctor and see what the cancer expert(s) can offer you.
- I have done my best for you – for the pasts 12 years – and now, I don’t have any more herbs to make your problems go away.
- Ina said the oncologist wanted her to do a biopsy and PET scan and most probably follow up with oral chemo or immunotherapy drugs.
- To be fair to Ina, I told her I am not going to give my opinion on this – she will have to make that decision herself. If that is the only route to take, just give it a try.
- I may give my thoughts but you and your family must come together, discuss and decide what to do.
- I asked Ina to take Lung Phlegm tea together with the Lung tea. This was to help her with the laboured breathing. It was indeed surprising that Ina told us she became normal again after taking this tea. I talked to her over the phone. Her voice was strong like any healthy person.
- I received these messages:
- 28 March 20240: Agreed to go for scan today. Letrozole + ribociclib. She still felt breathless the whole day. Couldn’t sleep the whole night again. I think she’s going to give it a try.
- 29 March 2023: Started on Letrozole and abemaciclib tonight. Biopsy confirmed hormone positive breast cancer.
- 2 April 2023: Im and I visited the Funeral Parlor to pay our last respect to Ina. We were told the following by various family members.
- Before Ina went to the hospital for the biopsy and treatment she was still okay. She was in her shop giving instructions to her staff on what to do.
- Ina was prescribed 2 oral drugs.
- Letrozole or Femara. This is a commonly prescribed oral drug for breast cancer patient. If you wish to know what this drug can do to a patient, click this link: https://cancercaremalaysia.com/2019/12/30/rotten-breast-suffered-after-three-weeks-on-letronat/
- A targeted therapy cancer drug (either abemaciclib (Yulareb or Verzenios) or ribociclib (Kisqali). I am not able to confirm which drug was being used. Anyway, these are new drug that are not readily available in most hospitals in Malaysia. This is the second time I have heard of abemaciclib being used on breast cancer patients. The first time was from a Indonesian lady. She had many cycles of this drug in Jakarta. Unfortunately, the result was disappointing. As for ribociclib, this is the first time that I heard of this drug.
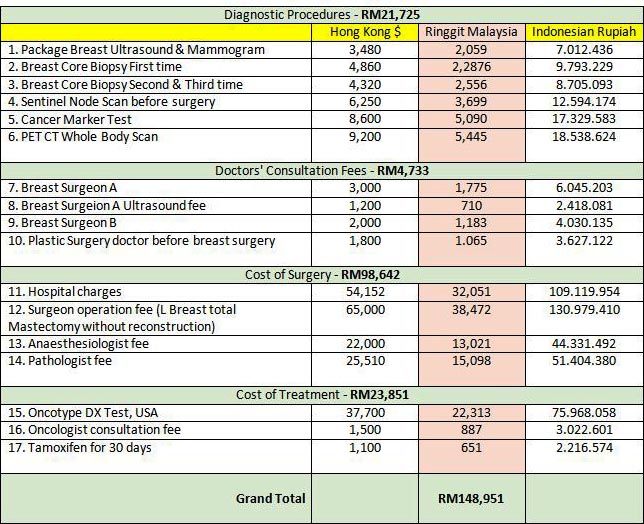
- According to Ina’s husband Ina was given a cycle of these drugs (plus other pills) and that costs RM90,000 (ninety thousand ringgit). The family was also told that should Ina needed to be admitted in the ICU, it would cost the family at least RM5,000 per day.
- Ina took the targeted therapy drugs:
- Day 1, Ina took 1 pill.
- Day 2, she took 2 pills.
- Day 3, she took 1 pill.
- Ina developed difficulties and she died early morning the next day, about an hour after the family had left the hospital for home.
Comments
Probably the first question anyone may want to ask is:Why did Ina die so fast? Three days after swallowing these scientifically proven drug, she was dead.
Can this be due to the following?:
- Her breast cancer which she had been living with for the past 12 years without any problem suddenly turned aggressive and killed her within 3 days. Can this ever happen?
- It is because of lung complications arising from her covid-19 infection.
- It is because of the scientifically proven targeted chemo drugs that she took?
- Oh, it is just her fate – just that her time is up.
I would not wish to give my comment on the above reasons. It is up to you readers to come to your own conclusion based on your belief. I cannot and would not want to change your belief system either. So be it.
By bringing up the above question, I am also not trying to ask you to find a scape goat either. The doctors did their best based on the knowledge that they had learned. All family members gave advices, rightly or wrongly, in the hope that what they said might help Ina.
To me, by sharing with you Ina’s story, is to highlight some lessons we can learn from Ina’s experience. Do you learn anything after reading her story?
Let me tell you what I learned. I thought, throughtout these 12 years, I have done my best to help Ina. But I must admit, upon reflecting on Ina’s case again, I would say I could have done better. I did not prescribe her the covid herbs that we have – especially the tea to deal with long covid symptoms. Yes, I gave Ina the lung herbs to help her with her lung problems but I wondered, could the covid herbs be better for her? To me, I believe the problem that Ina was facing was not breast cancer – she had been living with this for the past 12 years!. Yes, the lung has breast cancer cells but what mattered most was that her lungs needed help – she had severe breathlessness, lack of energy or strength, etc. Could these be caused by the covid infection she had earler – the monster referred to as long covid?
To understand more, visit the NHS, UK website: https://www.nhs.uk/conditions/covid-19/long-term-effects-of-covid-19-long-covid/
- How long does fatigue last after COVID-19? Your recovery from COVID-related fatigue will likely depend on how severe your illness was. After a mild case of COVID-19 your fatigue may clear up after about 2-3 weeks. But if you had a severe case, it’s possible to feel sluggish and tired for months.
Ina “recovered” from her covid infection but her problems did not go away for many months. After recovering from covid, Ina took time off to visit South Korea. When she came home (according to her husband), she was still coughing.
More from the internet ….
- Long COVID still worrisome 2 years after infection – even two years after infection with the virus, fallout from COVID-19 may persist.
- COVID-19 can cause lasting lung damage.
- Covid-19 continues to harm the body even months after a seeming recovery
- Long COVID Has Caused Thousands of US Deaths: New CDC Data
- COVID-19 can cause lasting lung damage.
What’s the link between coronavirus and lung cancer? COVID-19 disproportionately harms frail persons, including the elderly, and those with comorbid conditions, including cancer patients who are immunocompromised.
Some people with cancer are at increased risk of serious illness if they get COVID-19, because their immune systems have been weakened by the cancer and/or its treatments.
What happens if cancer patients get COVID? Studies show that having a history of cancer may also increase your risk of serious illness and death from COVID-19.
Why is COVID bad for your lungs? After a COVID infection, the immune system can inflict remote damage on other organs by triggering serious inflammation throughout the body – and this is in addition to damage the virus itself has directly inflicted on the lung tissue.
Is there a problem with lung after COVID? If COVID-19 pneumonia progresses, more of the air sacs can become filled with fluid leaking from the tiny blood vessels in the lungs. Eventually, shortness of breath sets in, and can lead to acute respiratory distress syndrome (ARDS), a form of lung failure.
What organs are affected by COVID? The virus that causes COVID-19, can damage the lungs, heart, brain, kidneys, and blood vessels. Inflammation was first thought to be the main source of this damage.
Does Covid stay in your body forever? Scientists at the University of California San Francisco have discovered that remnants of the COVID-19 virus can linger in blood and tissue for more than a year after a person is first infected.
Does COVID weaken your immune system? In a small study supported by the National Institute of Allergy and Infectious Diseases (NIAID), severe cases of COVID-19 were shown to cause long-lasting changes to the immune system.
What are long Covid lung symptoms?
- Difficulty breathing or shortness of breath.
- Cough.
- Chest pain.
- Fast-beating or pounding heart (also known as heart palpitations)
- Trouble breathing.
- Persistent pain or pressure in the chest.
- Inability to wake or stay awake.
Death is Not a Failure
Many people often time believe that to die is a failure. This idea is notoriously perpetuated in medicine.
Dr. Robin Kelly (in Healing Ways) said: Fear of death is seen as a necessary part of modern medicine … This idea stems from a materialistic view about life.
Dr. Bernie Siegel wrote: I experienced being unhappy as a doctor. I was uncomfortable with the mechanical approach that we are taught in medical school. My success is measured by whether or not I saved your life. If I can’t save your life, I’m a failure. But now I don’t feel like a failure. I can help you live. After all you’re not going to live forever, no matter what I do.
Those who are spiritually orientated understand that life on earth is only transient and therefore view life and death in a different light. There is an Indian saying: When you are born, you cried and the world rejoiced. Live your life in such a manner that when you die, the world cries and you rejoice.
To me, this is the secret of how we can triumph and give meaning and beauty to our own death. We can leave this world with a sense of pride and dignity knowing that we have done our best to make it a slightly better place for those we leave behind.
I saw Ina lying in the coffin and was told that the white blouse that she wore was specially designed by her. I believe Ina was well prepared for this day. I am sorry I cannot make her live for the next “thirty years” but she had done 12 years very well. Being a business woman Ina had many customers who had cancer. They went through surgery, chemo, radiation, tamoxifen, etc. Many suffered from the treatment and some died.


I recall what Ina told me after she went to consult the oncologist for her problems. Ina said something to this effect: The doctor was surprised. He said: You have stage 4 cancer and you can walk into my office like a normal person! Generally, stage 4 patient come in a wheelchair looking very sick. You walk in like a healthy lady with no problem!
No, Ina’s death is not a failure.
Let me end with what Dr. Bernie Siegel wrote in Peace, Love & Healing:
- It is important that we realize that we can never cure everything. We will never find … cure for all the diseases. Dying can be a healing, ending a full, rich life for someone who is tired and sore and in need of rest.














































You must be logged in to post a comment.