On the last day of 2017, I received an email from a Malaysian lady in Germany. Let’s call her May. This is what she wrote:
Dear Mr. Chris Teo,
…. I would like to tell you a bit about my case. All our reports are in German. We will translate them and bring them back to you.
- December 2016: I was diagnosed with undifferentiated pleomorphic sarcoma at blood vessels, which was near to my heart. The tumor grew from my right upper pulmonary vein through the mitral valve into my left ventricle of my heart. Via complete sternotomy, the tumor was excised.(Sternotomy — surgery where sternum or breastbone in centre of chest was divided or cracked).
Sternotomy was done one more time to stop internal bleeding and to remove a hematoma.
- January – June 2017: Cytostatic chemotherapy was done with Doxorubicin and Ifosamid for 6 cycles.
- October 2017: From standard checkup (CT scan and MRI), it was confirmed that a tumor, 2.4 x 2.2 cm is growing close to the right upper pulmonary vein and it presses onto the vein.
This result highly indicates a local recurrence. Sample of the tumor was taken via Endobronchial Ultrasound to pathology and it was confirmed it is the same high graded sarcoma.
- November – December 2017: Chemotherapy (Gemcitabin and Docetaxel) for 2 cycles were done. Along with the chemotherapy, I took part in a double blind clinical study for Antibodytherapy Olaratumab).
During chemotherapy and antibody therapy the tumor had shrunk to 1cm (result from a CT scan).
- 27 December.2017:A CT scan of the whole body was done and metastasis was found in my brain. It was located above my left eye.
- 2 January 2018: It is planned now to remove the tumor, as the tumor has caused brain edema which can cause stroke or bleeding anytime.
If the recovery process and the operation turns out successful and I still can fly, we will come back to find you to try your method to control the primary tumor near my heart.
Regards.
This was my reply to May.
Thank you for your email. Actually I was wondering who you are and why you want to come and see me. You are from Germany and I am in Malaysia, half a world away.
Since Netherlands is so near you, why don’t you see Dr YY below. You can get her contact from the internet. I have read her 2 books but I have never met her personally. But that is the way to start … see her and ask for her advice.
I also know Germany is very famous for alternative cancer therapy — why don’t you scout around to go to these clinics — if you need help to find where and what, let me know. I may be able to help.
Sarcoma is a very difficult problem … see, even chemo and chemo … did not work. You asked to see me in Penang — you are welcome to see me. Are you from Penang?
Dear Mr Chris Teo,
I am from Kedah. If I am fit and the operation goes smoothly, I will come and meet you. Thank you and Happy new year.
In early February 2018, May, her husband and her mother came to our center.
May was prescribed a variety of herbal teas for her brain and sarcoma. Once in a while, I received updates of May’s progress.
Hello Uncle Chris,
8 Feb: I started soft tissue tea. My thigh has less pain. A bit pain at my left chest.
9 Feb: I feel some short pain at my left chest. When I first swallow food or water, my tracea is pain.
10 Feb: Same like 9.2
11 Feb: My thigh is less pain. But still pain when I swallow food or water.
12 Feb: My thigh still has a bit pain. Still pain when I swallow food and water.
13 Feb: still pain when I swallow food and water.
14 Feb: My cheek and neck is itchy and red. My thigh has no more pain.
15 & and 16 Feb: My cheek and neck still itchy and red. Still a bit pain when I swallow food.
17 Feb: No more pain when swallow food or drink water. My cheek and fore head are still itchy and red.
18 Feb: Still itchy at fore head and cheek.
19 Feb: Light pain at my left chest. A bit hard to explain.
On 28 March 2018 May, her husband and mother dropped by the centre before returning to Germany. And while in Germany May did write once a while to update us.
On10 May 2018, this is what she wrote:
Hello Dr.Teo,
I have check up and it shows that the tumour has reduced its size to half and no metatasis. A very big thanks to you from me and my whole family. My oncologist here in Germany is so curious about my therapy and would like to know more. So I gave him your website. They haven’t see such improvement before with chemo and radiation especially with my rare sarcoma. Thank you once again.
Reply: You wrote: I have check up and it shows that the tumour has reduced its size to half and no metatasis.
Can you tell me what does this mean? Before the herbs you have tumour ? Where? What is the size?
Now, what did the doctor do? CT or MRI … then what is the size?
10 May 2018:
Dear Dr.Teo,
I had recurrence before I came to see you. The primary tumour is located in the lymph node near my heart. The cancer metatasized to my brain. When I first met you in January. The doctor had removed the tumour in the brain but not the primary one.
The primary tumour in December was 5.5 x 3.2cm. Now it has become 3.2 x 1.9 cm.
Comments
- When I received May’s email, my first reaction was to ask her to see other alternative healers — Germany is so famous for alternative medicine — why come to CA Care? But since she insisted of following our therapy, I could not turn her down. Perhaps she missed “home” too. Good to be back in your own “kampong” and be among your loved ones when you are ill — right?
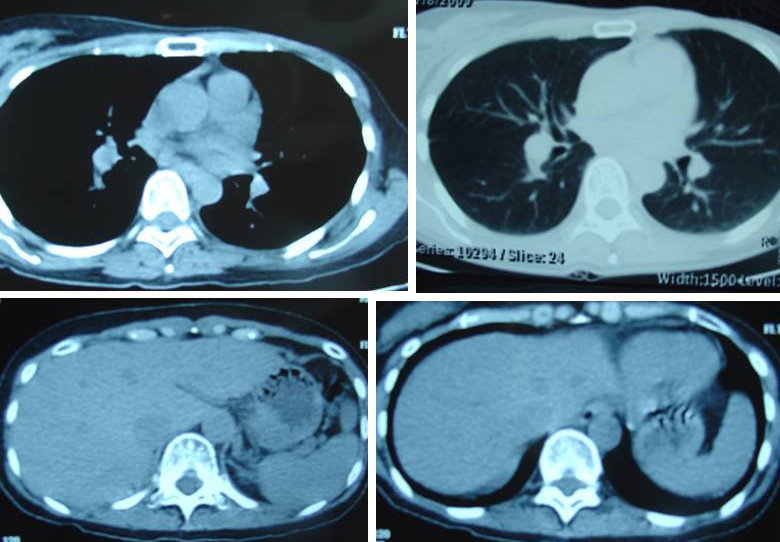
- Below are pictures of the mass around her heart (top) and a tumour in her brain (below). After seeing this I shook my head in despair. As I told May, in my twenty plus years helping cancer patients, this is my first time seeing such a cancer. I really don’t know what I can offer May. But as you can see from this report, the herbs gave very encouraging results.
Sarcoma in blood vessel around heart
Sarcoma spread to brain.
Note: Undifferentiated pleomorphic sarcoma (UPS), is a type of soft tissue cancer. The word “undifferentiated” means that the cells don’t resemble the body tissues in which they develop. The cancer is called pleomorphic because the cells grow in multiple shapes and sizes.
While sarcomas are rare tumors, they do represent one of the most common soft tissue malignancies in adults. Soft tissue sarcomas can develop in blood vessels and in deep skin, fat, muscle, fibrous or nerve tissues. The cancer typically becomes quite large over a period of weeks or months, sometimes growing quite rapidly. The cancer can spread to other locations in the body, most often the lungs.
- May told her German doctor that she wanted to come home to undergo our therapy. The doctor did not object to her taking herbs! After all the doctors in Germany had done their best — even surgery and chemotherapy failed — what else could they offer her except more of the same treatments.
From the start, I make it clear to May that I would not be able to cure her — to help her, probably yes. I know sarcoma is a very difficult cancer to handle. But, right in my head, I know that I had some wonderful successes with sarcoma. Read these stories if you want to know more: https://cancercaremalaysia.com/category/sarcoma/
- Now that the tumour has shrunk rather significantly, just after three months of herbs, I pray that things become better and better with time. But May will have to help herself. She should keep on doing what she has been doing after seeing us. Don’t ever think that she can do and eat anything she likes!
- This statement that May wrote, My oncologist here in Germany is so curious about my therapy and would like to know more, tickled me a bit! Most doctors/ oncologists generally don’t want to know! If you don’t want to know you are like “a frog under the coconut shell”, right?
- I must say frankly, I would not know what is May’s future but for what it is we need to lift up our eyes to Heaven and praise the Almighty God for this healing. God bless.































You must be logged in to post a comment.