It was 3 a.m. when I finished reading the last page of this 224-page-New York Time #1 Bestseller.
The Author: Dr. Paul Kalanithi was an outstanding neurosurgeon with very impressive academic credentials. He graduated from Stanford University with a BA and MA in English literature and a BA in human biology. He earned an MPhil in history and philosophy of science and medicine from the University of Cambridge. Later, he went to Yale School of Medicine where he graduated with a cum laude. Paul then returned to Stanford to complete his residency training in neurosurgery.
To Paul, being a neurosurgeon is a noble calling. You can’t see it as a job, because if it’s a job, it’s one of the worst jobs there is.
Unfortunately, fate has it that Paul did not end up being a full-fledged neurosurgeon. Well into his six-year-residency he was diagnosed with stage 4 metastatic lung cancer. Less than two years (22 months) after the diagnosis he died — just when he was ready to graduate.
I read this book with a heavy heart — sad that such a brilliant and caring doctor like Paul had to leave so soon. Lucy — Paul’s wife wrote, When I see the hospital where Paul lived and died as a physician and a patient, I understand that had he lived, he would have made great contributions as a neurosurgeon and neuroscientist. He would have helped countless patients and their families.
Such is the sad, cruel reality about life. Lucy wrote, What happened to Paul was tragic, but he was not a tragedy. True indeed. I always believe for anything that happens, there must be a reason if only we look at the bigger picture.
Salute the Neurosurgeon!
Paul did well in life — he studied literature, history and philosophy before doing medicine. With such academic background he was well prepared to become a caring doctor — a cut above others. Here are some quotations of what Paul wrote in his book:
- As a resident, my highest ideal was not saving lives — everyone dies eventually — but guiding a patient or family to an understanding of death or illness. Where there’s no place for the scalpel, words are the surgeon’s only tool.
- Our patients’ lives and identities may be in our hands, yet death always wins. Even if you are perfect, the world isn’t. The secret is to know that the deck is stacked, that you will lose, that your hands or judgment will slip, and yet still struggle to win for your patients.
- Like my own patients, I had to face my mortality and try to understand what made my life worth living. With limited time, Paul wrote this book. He did not get to finish it.
Prognosis and Statistics
As a neurosurgery resident Paul had operated on brain cancer. After surgery it is the standard practice to send patients for follow up chemo and/or radiation. Here doctors often talk about prognosis with their patients and family members.
This is something Paul wanted us to know. He wrote, By this point, I had learned a couple of basic rules. First, detailed statistics are for research halls, not hospital rooms … Second, it is important to be accurate, but you must always leave some room for hope — Median survival is eleven months or You have 95 percent chance of being dead in two years — I come to believe that it is irresponsible to be more precise than you can be accurate. Those apocryphal doctors who gave specific numbers (The doctor told me I had six months to live): Who were they, I wondered, and who taught them statistics?
Limitation of Science
- Although I had been raised in a devout Christian family …I, like most scientific types, came to believe in the possibility of material conception of reality, an ultimately scientific worldview that would grant a complete metaphysics, minus outmoded concepts like souls, God, and bearded white men in robes.
- Scientific methodology is the product of human hands and thus cannot reach some permanent truth. We build scientific theories to organize and manipulate the world, to reduce phenomena into manageable units.
- Science is based on reproducibility and manufactured objectivity.
- Science … its inablity to grasp the most central aspects of human life: hope, fear, love, hate, beauty, honor, weakness, striving, suffering, virtue.
- Human knowledge is never contained in one person. It grows from the relationships we create between each other and the world, and still it is never complete.
Stage 4 Lung Cancer
- At age thirty-six, I had reached the mountaintop; I could see the Promised Land …. then a few weeks later I began having bouts of severe chest pain … my weight began dropping … from 175 to 145 pounds. I developed persistent cough. Little doubt remained.
- In May 2013, it was confirmed that Paul had a stage 4 non-small cell EGFR-positive lung cancer. At that time he was in his sixth year of residency — one more year to
- The irony was that Paul had never smoked.
The World’s Best Oncologist
- The search was on — to find who was the best lung cancer oncologist (USA). Houston and New York had major cancer cancers …The replies came back quickly and more or less unanimously: Emma (also in Stanford) not only was one of the best — a world-renowned oncologist who served as the lung cancer expert on one of the major national cancer advisory boards — but she was also known to be compassionate, someone who knew when to push and when to hold back.
- On many occasions when consulting Emma, it was clear that this compassionate oncologist did not “dictate things” to her patient. I could hear Emma’s voice again: You have to figure out what’s most important to you.
- Emma once told Paul: I’m totally happy for us to make your medical plan together; obviously, you’re a doctor, you know what you’re talking about, and it’s your life.
- At their initial consultation, Paul wanted to discuss the prognosis — possibly how much time left. Emma evaded the question and said, We’re not discussing that.
- Two months in, Emma remained vague about any prognostication, and every statistics I cited she rebuffed with a reminder to focus on my values.
Temporary Response
Paul had an EGFR-positive tumour. No intravenous chemotherapy was indicated for the moment. He was put on an oral targeted drug called Tarceva.
His cancer responded to the treatment — My lungs, speckled with innumerable tumours before, were clear except for a one-centimetre nodule in the right upper lobe … there had been a clear, dramatic reduction in tumour burden.
Paul regained strength and he returned to work in late 2013, completing his seventh year of residency.
Relapse — Chemotherapy: Too many cooks spoil the broth?
In spring of 2014, the cancer relapsed. The only option left was chemotherapy. This was what happened after one of his chemo sessions.
- I began to deteriorate, my diarrhea rapidly worsening … my kidneys began to fail. My mouth became so dry I would not speak or swallow … my serum sodium had reached a near-fatal level. Part of my soft palate and pharynx died from dehydration and peeled out of my mouth … I was transferred to the ICU. I was in pain …. a pantheon of specialists was brought together to help: medical intensivists, nephrologists, gastroenterologists, endocrinologists, infectious disease specialists, neurosurgeons, general oncologists, thoracic oncologists, otolaryngologist ….
- I was acutely aware that with this many voices, cacophony (unpleasant mixture of loud sounds) In medicine, this is known as the WICOS problem: Who Is the Captain Of the Ship? The nephrologists disagreed with the ICU doctors, who disagreed with the endocrinologists, who disagreed with the oncologists, who disagreed with the gastroenterologists. I felt the responsibility of my care… tried to corral all the doctors to keep the facts and interpretations straight.
It is hard to tell laymen, like you and me, to take charge of your own health and treatment when you are in the hospital surrounded by all those experts. But yet, that should be the way it should be!
Chemotherapy took a heavy toll on Paul. He wrote: Withered, I could see my bones against my skin, a living X-ray. At home, simply holding my head up was tiring. Lifting a glass of water required both hands. Reading was out of question.
Chemo Failed – He Died
- Treatment wasn’t an option — not until I regained some strength.
- Emma, I said, what’s the next step?
- Get stronger, That’s it.
- But when the cancer recurs … I mean, the probabilities …. I paused. First-line therapy (Tarceva) had failed. Second-line therapy (chemo) had nearly killed me. Third-line therapy, if I could even get there, made few promises.
- You have five good years left, she (Emma) said. She pronounced it, but without authoritative tone of an oracle, without any confidence of a true believer. She said it, instead, like a plea… Doctors, it turns out, need hope, too.
Paul did not live to write the closing chapter of his book. It was left to his wife, Lucy, to document his last hours on earth in the Epilogue. Paul died, two months short of two years (on Monday, 9 March 2015) after his diagnosis. He was 37 years old.
- In the Epilogue Lucy said, Writing this book was a chance for this courageous … (Paul) to teach us to face death with integrity.
To us who is still living, I also say, Let us learn to embrace death with courage and understanding.
Lessons from Paul’s Experience
As I read this book, I learned many things. And I kept thinking and asking. Let me share my thoughts with you.
Family of Doctors
Paul came from a family of doctors. His father, brother, uncle, wife are all doctors. Paul was not any ordinary doctor. He was trained in one of the best medical schools in the country. When he had cancer, he had the best oncologist in the world to treat him. Few of us would not have that privilege and opportunity. Perhaps we don’t need the best when it comes to cancer? What difference would that make?
Modern medicine had contributed very much to lighten human sufferings. Let no one doubt about that. But when it comes to cancer and its treatment, perhaps we need to take a step backward, pause and explore more.
Yes, many people wrote about the need to rethink the war on cancer, but there are many others who would strongly defend the status quo. Why change? Why look for something else when the present ways serve the Cancer Industry so well?
When my wife and I started CA Care in 1995, to help cancer patients, I knew absolutely nothing about cancer and its treatment. No, I did not go to medical school. I relied on my Ph.D. and my research experience on plants to do what is right for those helpless and hopeless patients. After 20 years of dealing with cancer patients, I can say this to all and sundry. As far as cancer treatment is concerned, there are other options than just chemo and radiation. Perhaps by taking the non-conventional path, you could live longer, with less suffering and not having to deplete your life’s saving to pay for the medical bills.
I have written numerous studies in these two comic books.
Available at http://bookoncancer.com/productDetail.php?P_Id=75
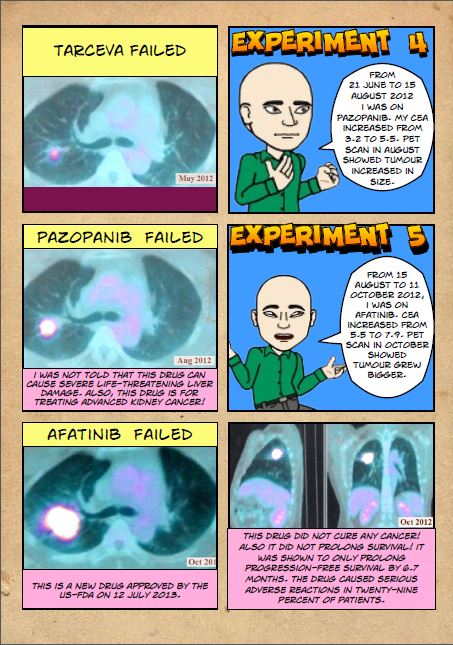
In Lung Cancer – What Now? I have documented 12 cases of lung cancers – nine of which are about patients who failed to find the cure that they wanted, in spite of spending hundreds of thousands of ringgit on their medical treatments.
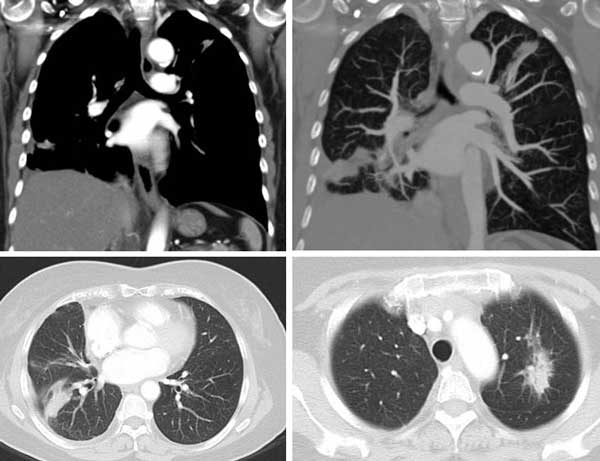
Meaningless shrinkage of tumour by Iressa
Meaningless shrinkage of tumour by Tarceva
These two cases happened with patients in Jakarta (above) and in Malaysia (below). And this also happened some years later with Dr. Paul in Stanford. What can we learn from such cases?
Available: http://bookoncancer.com/productDetail.php?P_Id=73
In Lung Cancer – Success Stories, I presented 12 cases of patients who opted for “alternative” treatment for their lung cancer.
Statistics of Lung Cancer Survival
Dr. Paul had Tarceva. This drug helped him for about a year. Then the cancer came back again. He then had chemotherapy and died. He survived 22 months after his initial diagnosis. That happened in Stanford under the care of the best oncologist in the world.
Back in Malaysia, there is also a professor who is the best for lung cancer. According to him, most of his patients who were treated in his clinic died after two years.
The same achievement as in Stanford?
If you do the same thing over and over again. You can expect the same results. Is that not what science teaches us? Remember what Henry Ford and Einstein said.
In this story above, mom opted for CA Care Therapy. She declined chemotherapy even though she was told that without chemo she would die within six months. Professor X was surprised how mom had survived for four years without chemo. Is that an achievement or quackery (like many in the medical industry want us to believe)?
Why haven’t you die yet?
CA Care has been around for about 20 years now. Like Dr. Paul, my wife and I went into this because it was a “calling” — an answer to my prayer. Looking back, we have no regrets. Instead, we feel blessed to be able to help patients who need our help. They come from far and near.


































































You must be logged in to post a comment.