FY is a 50-year-old Malaysian. His problem started with headache, poor appetite and weight loss. He consulted a doctor in a private Hospital A in his hometown. He was told there could be something in the brain. A CT scan was done and there was a lump in his lung. A biopsy confirmed a moderately differentiated adenocarcinoma.
FY was referred to a private Hospital B in Penang. The biopsy tissue was sent to Kuala Lumpur for further analysis. EGFR mutation was detected. In the meantime, FY underwent five times of radiation to the head (due to the headache). This treatment cost RM11,000. The oncologist suggested taking oral chemo.
FY decided to seek further treatment in another private Hospital C. The oncologist in Hospital C prescribed oral drug, Tarceva. This was the deal. Take Tarceva for ten months, thereafter it will be provided free of charge for life. Each month’s supply cost RM4,500, meaning FY will have to fork out a total of RM45,000 first before he could enjoy the free supply of Tarceva.
In all, FY took Tarceva for 11.5 months. So, he managed to enjoy free Tarceva for 1.5 months.
Medical Reports
The progress of FY’s treatment was monitored by scanning and blood tests.
CT scan thorax done in Hospital A, 29 August 2017.
- a suspicious 3.4 x 2.8 x 3.3 cm lump in the lower lobe of his left lung.
CT scan of brain, neck, thorax, abdomen and pelvis done in Hospital C, 26 September 2017.
- lesion at apical segment of left lower lobe of lung and small cavities due to primary carcinoma.
- multiple small metastases in both lungs.
- enhancing lesions at left parietal lobe, vermis and right cerebellum.
- patchy sclerosis of body of T1 vertebrae suggestive of metastasis.
- lymph node at level 4 of neck.
MRI thoraco-lumbar spine done in Hospital C, 3 October 2017.
- abnormal signal intensity within C7,T1 and T2 vetebral bodies. Features suggestive of metastases.
- L4/L5 disc bulge.
- L5/S1 disc bulge.
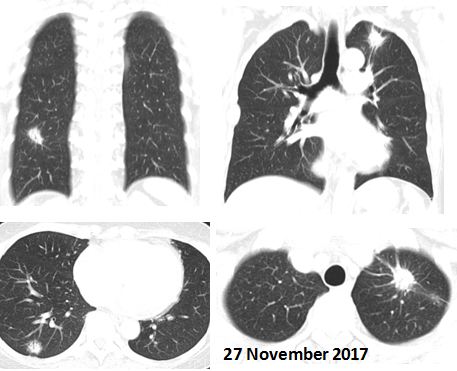
Whole body PET Scan done in Hospital C, 18 January 2018.
- metabolic activity noted in the right (1.8 cm) and left sides of neck (1.9 cm) .
- metabolic activity noted in the left base of the tongue.
- metabolic activity left axillary lymph node (2 cm).
- irregular metabolic active mass (3.2 cm) seen in the apical segment of the lower lobe of left lung.
Whole body PET Scan done in Hospital C, 21 August 2018.
- metabolic activity node see in the left (1.3 cm) side of the neck.
- metabolic activity left axillary lymph node (0.6 cm).
- FGD-avid mass (4 cm) seen in the apical segment of the lower lobe of left lung. This is larger and has more metabolic activity compared to the previous PET CT on 18 Jan. 2018.
- metabolic active nodule (1.9 cm) seen in the posterior segment of the upper lobe of right lung – not seen in the previous scan.
- another metabolic active nodule (1.7 cm) seen in the posterior basal segment of the lower lobe of the left lung — not seen in the previous scan.
- a few 2-5 mm, non metabolic active nodules seen in the right and left lungs. These are not seen in the previous scan.
- increased metabolic activity seen in the left adrenal gland (1.4 cm).
- metabolic active lesions seen in the spine of C7 and T1. These re larger and more metabolic active compared to the previous PET CT scan.
- metabolic active bony lesions seen in the spine T12, left sacrum and medial wall of the left acetabulum. These are not metabolic active in the previous scan.
You don’t need to be a doctor to know that FY is getting worse, not better, after taking Tarceva.
Below is a table with values of CA125, CA15.3 and CA19.9 taken over a period of about a year while FY was taking Tarceva. The most telling results are the values of CA125. In September 2017, the value was 434. After taking Tarceva it gradually decreased to 48 and down to 15 in February. But in March 2018 (barely five months later) the CA125 started to increase and in August 2018 it was at 46.5.
| Date | CA 125 (0-35) | CA 15.3 (0-31.3) | C19.9 (0-37) |
| 26 September 17 | 434 | 9.8 | 39.4 |
| 24 October 17 | 48 | 7.7 | 16.9 |
| 28 November 17 | 15 | n/a | n/a |
| 27 December 17 | 15 | n/a | n/a |
| 23 February 18 | 15 | 4.9 | 8.2 |
| 26 March 18 | 18 | 5.8 | 15.6 |
| 23 April 18 | 19 | 5.9 | 11.0 |
| 22 May 19 | 22 | 5.2 | 17.0 |
| 25 July 18 | 40.6 | 5.1 | 17.2 |
| 17 August 18 | 46.5 | n/a | n/a |
The numbers above clearly showed that Tarceva was gradually losing its effective after five months!
In August 2018, the oncologist told FY that Tarceva was not effective anymore. He has to switch to i/v chemotherapy and radiotherapy. A cycle of chemo would cost RM12,000.
If FY does not want chemo, he can opt for another new, more expensive oral drug (probably Tagrisso which cost RM30,000 per month).
FY and his wife came to seek our help. They decided not to continue with further medical treatment – at least for the moment.
Chris: Can this new drug cure you?
FY: No, only control.
Comments
This my third case in which patients were asked to take Tarceva for ten months with the promise that at the 11th month onwards they get Tarceva without charge for life!
Do you ever wonder why patients are offered Tarceva for free, after being told to buy a ten-month- supply first? Is it a noble, charitable intention or “smart” business deal?
Read this story: Lung Cancer: Spend RM80,000 and You Get Free Tarceva for Life
Daughter: My father has lung cancer. It is positive for EGFR. The doctor suggested taking the oral targeted therapy, Tarceva. One box, lasting one month, cost about RM8,000. After we take Tarceva for ten months, and if the medicine works, for the rest of his life the medicine will be free. But must complete the ten boxes first. That’s the deal!
Chris: You mean after spending RM80,000 they will give you Tarceva for free for life? But what happen if your father dies before the ten months?
D: I was thinking. May be my father cannot last that long. Maybe before the ten boxes, sure die one.
C: I have one patient who came and see me. She was asked to take Nexavar (for liver cancer). The deal was buy one, free one. But must pay RM20,000 first (for the first month’s supply) and next month she will get one month’s supply of Nexavar for free! But after she took the drug for a week, her health deteriorated, had to be hospitalised and she died. Already paid RM20,000, cannot claim back.
Another question that bugs me is, why free only after TEN months? Why not earlier? Why not buy one, free one like they offered for Nexavar?
Let’s study the blood test numbers critically. Let’s look at the bigger picture. The CA125 was at 434 in September 2017. After taking Tarceva the value dropped to 15. Bravo! Tarveca seemed to do the magic. But this euphoria did not last long. A month later, in March 2018, the CA125 started to increase. By August 2018, it was at 46.5.
By offering patients free Tarceva after ten months, seems appealing and noble at the first look; but in reality does the drug company or doctor not know that by a few more months, patients don’t need Tarceva anymore because it is not effective?
From a business point of view, it also does not make “sense” why the drug company would give Tarceva for free. Business is to make money. Just imagine what could happen if all patients get free Tarceva for life — will that not make the drug company go bankrupt?
Let me share with you what my favourite Jewish rabbi, Harold Kushner said:
When I started to ask these questions, I became more curious. To kill the curiosity in me, I googled cost of generic Tarceva in India.
This is what I get.
- In many countries, the brand-name Tarceva 150 mg drug costs about $18,700to 19,000 (price subject to vary) per 30 tablets. However, the mass production of generic cancer drugs versions are available for less than 15% of the retail price of the brand-name drug. Mar 22, 2018
Click this link and you get prices of generic Taceva available in India
https://dir.indiamart.com/impcat/erlotinib-tablets.html
(Exchange rate: Indian Rupee 10,000 = RM 563)
In India you can buy a month supply of generic Tarceva for less about RM563. Wow, amazing — I learned something new today! At one time Tarceva was selling for RM 8K per month. Now the price dropped to RM5K — and that is still many times more expensive than the Indian generic.
Erlotinib Rs 11,900, 150 mg, 30 tablets
Erclocip Rs 7,230 for 30 tablets
Erlonat Rs 6,000 for 30 tablets
Erlonat by NATCO,Rs 10,000 for 30 tablets
I have another question. I wonder why the Power-that-Be in developing countries do not look to India for the cheaper, generic drugs? Is that not a good way poor for poor countries to save money?
If you are skeptical about this suggestion, that is okay. Go ahead and spend your money.
But if you are poor and cannot afford to buy these expensive, American drugs, I believe my suggestion makes sense.
Take this case, FY paid for the “expensive original” Tarceva, right? For less than a year, he already spent RM45,000. Look what happened to him?
Go to these links and read:
Generic cancer drugs that we can trust
Access to cancer medicines in India
India to supply generic cancer drug to US
India approves generic cancer drug
Dying to Survive: Indian generic medicines have a tale to tell
Terminally ill dad saves more than $200k bringing in cancer drugs from India





































































You must be logged in to post a comment.