Ria is a 53-year-old lady from Jakarta. About four years ago she was diagnosed with breast cancer and had a right mastectomy at a private hospital in Penang. Since she did not bring the medical report of her surgery, I was not able to tell you how serious her breast cancer was. Anyway, Rias was asked to undergo follow-up treatments — chemotherapy and radiotherapy. She refused. She was not on any medication either.
Ria was okay after the surgery and did not bother to come back for any check-up after that. About three months ago (i.e. about four years after her mastectomy), Ria became breathless. She was admitted to a hospital in Jakarta and was told there was fluid in her lungs. The doctor wanted her to undergo chemotherapy. She refused.
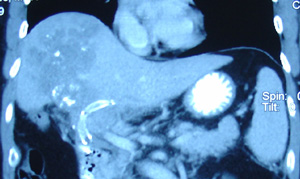
Ria came back to the same private hospital in Penang where she had her surgery. She was referred to the lung specialist. A CT was done and showed the following:
- There is a 5.5 x 5.1 x 3.5 cm mass in the manubrium sterni with an extension of the mass into the prevascular space of the mediastinum.
- There is moderate to large right pleural effusion (fluid in the lung).
- Collapse-consolidation of right lower lobe.
- Right and left main pulmonary arteries and their lobar branches are consistent with pulmonary embolism (PE).
Ria’s right leg was swollen and USG confirmed it was due to extensive deep vein thrombosis (DVT) of the right common femoral, superficial femoral and popliteal veins.
The lung specialist was not able to offer Ria any help and referred her to the oncologist instead. Ria was told to undergo 6 cycles of chemotherapy with Taxol and Epirubicin. She refused chemo.
From the pictures above, her breast cancer must have spread to her lungs, bone and liver. In addition she suffered DVT of the right leg. The doctor wanted Ria to be admitted into the hospital right away, to treat her DVT. She also refused.
Ria came to seek our help instead.
What can I do with such a case? Listen to our conversation that morning.
Three Weeks After Taking the Herbs
Ria came back to see us again. She was full of energy and was happy. Her swollen leg was almost (70 percent) healed. Before the herbs her right leg was “hot”, hard and painful. After taking the herbs, it was back to normal.
When Ria first came three weeks ago, I did not believe that I could do anything to help her. This was because I had a bad experience with DVT before. When we first started CA Care twenty plus years ago, I remember of a young man, an engineer, who had cancer and underwent chemotherapy. He developed DVT (deep vein thrombosis) in his thigh. His wife came to our house well after mid-night asking for help. I could do nothing for him. He immediately underwent an operation for his DVT and died.
I told Ria. “I am really surprised. When you first came three weeks ago, I did not write anything about your case history. See the blank page. This is because I thought your condition was so serious that you could die anytime. I did not expect you to live. I am glad that you are well now. God really loves you!”
Then jokingly I told Ria. Now that you are okay, why don’t you go for chemotherapy for your recurrent breast lumps. Ria replied, “Itu racun — that is poison”! What a surprising answer. Ria is not an educated lady. She makes kue — local cakes — to sell in Jakarta market. But she know what chemo is!
From the internet, I gather some information about DVT.
- Deep vein thrombosis, or DVT, is a blood clot that forms in a vein deep in the body. Most deep vein clots occur in the lower leg or thigh.
- Deep vein thrombosis can cause leg pain or swelling with red or discolored skin on the leg. There is a feeling of warmth in the affected leg. This is what Ria said she had.
- Deep vein thrombosis can be very serious because blood clots in your veins can break loose, travel through your bloodstream and lodge in your lungs, blocking blood flow (pulmonary embolism). And that is exactly what the CT scan showed Ria had: Right and left main pulmonary arteries and their lobar branches are consistent with pulmonary embolism (PE).
- A deep vein thrombosis canbreak loose and cause a serious problem in the lung, called a pulmonary embolism, or a heart attack or stroke.
- A pulmonary embolism can be life-threatening. Signs and symptoms of a pulmonary embolism include: sudden shortness of breath, chest pain or discomfort that worsens when you take a deep breath or when you cough, feeling lightheaded or dizzy, or fainting, rapid pulse and coughing up blood
Can DVT kill you?
- Yes, you can die of a deep vein thrombosis. If a pulmonary embolism(PE) occurs, the prognosis can be more severe.
- If the clotis big or the artery is clogged by many smaller clots, a pulmonary embolism can be fatal. About 25% of people who have a PE will die suddenly.
- In the US, every five minutes someone dies from a blood clot or deep vein thrombosis. Each year between 100,000-180,000 Americans die as the result of pulmonary embolism.



























































You must be logged in to post a comment.